Rethinavel et al., Journal of Chemical Neuroanatomy, 2021.05
“COVID-19 has been characterized by the degeneration of sensory neurons and dopaminergic neurons in the olfactory system.
SARS CoV-2 infection appears to be a risk factor for Parkinson’s disease (PD).
The impairment of neurogenesis in the olfactory system in COVID-19 and PD can be the potential cause of anosmia.
Neural regenerative therapeutics need to be considered for COVID-19.”
“Anosmia, a neuropathogenic condition of loss of smell, has been recognized as a key pathogenic hallmark of the current pandemic SARS-CoV-2 infection responsible for COVID-19. While the anosmia resulting from olfactory bulb (OB) pathology is the prominent clinical characteristic of Parkinson’s disease (PD), SARS-CoV-2 infection has been predicted as a potential risk factor for developing Parkinsonism-related symptoms in a significant portion of COVID-19 patients and survivors. SARS-CoV-2 infection appears to alter the dopamine system and induce the loss of dopaminergic neurons that have been known to be the cause of PD. However, the underlying biological basis of anosmia and the potential link between COVID-19 and PD remains obscure. Ample experimental studies in rodents suggest that the occurrence of neural stem cell (NSC) mediated neurogenesis in the olfactory epithelium (OE) and OB is important for olfaction. Though the occurrence of neurogenesis in the human forebrain has been a subject of debate, considerable experimental evidence strongly supports the incidence of neurogenesis in the human OB in adulthood. To note, various viral infections and neuropathogenic conditions including PD with olfactory dysfunctions have been characterized by impaired neurogenesis in OB and OE. Therefore, this article describes and examines the recent reports on SARS-CoV-2 mediated OB dysfunctions and defects in the dopaminergic system responsible for PD. Further, the article emphasizes that COVID19 and PD associated anosmia could result from the regenerative failure in the replenishment of the dopaminergic neurons in OB and olfactory sensory neurons in OE.”
Rebholz et al., Frontiers in Neurology, 2020.10
“The loss of the senses of smell (anosmia) and taste (ageusia) are rather common disorders, affecting up to 20% of the adult population. … Not only is olfactory dysfunction rather prevalent in the healthy population, it is, in many instances, also a correlate or an early indicator of a panoply of diseases. Importantly, olfactory dysfunction is linked to the two most prominent neurodegenerative disorders, Parkinson's disease and Alzheimer's disease. Anosmia and hyposmia (reduced sense of smell) affect a majority of patients years before the onset of cognitive or motor symptoms, establishing olfactory dysfunction as early biomarker that can enable earlier diagnosis and preventative treatments. In the current health crisis caused by SARS-CoV2, anosmia and dysgeusia as early-onset symptoms in virus-positive patients may prove to be highly relevant and crucial for pre-symptomatic Covid-19 detection from a public health perspective, preceding by days the more classical respiratory tract symptoms such as cough, tightness of the chest or fever. Thus, the olfactory system seems to be at the frontline of pathologic assault, be it through pathogens or insults that can lead to or at least associate with neurodegeneration. The aim of this review is to assemble current knowledge from different medical fields that all share a common denominator, olfactory/gustatory dysfunction, and to distill overarching etiologies and disease progression mechanisms.”
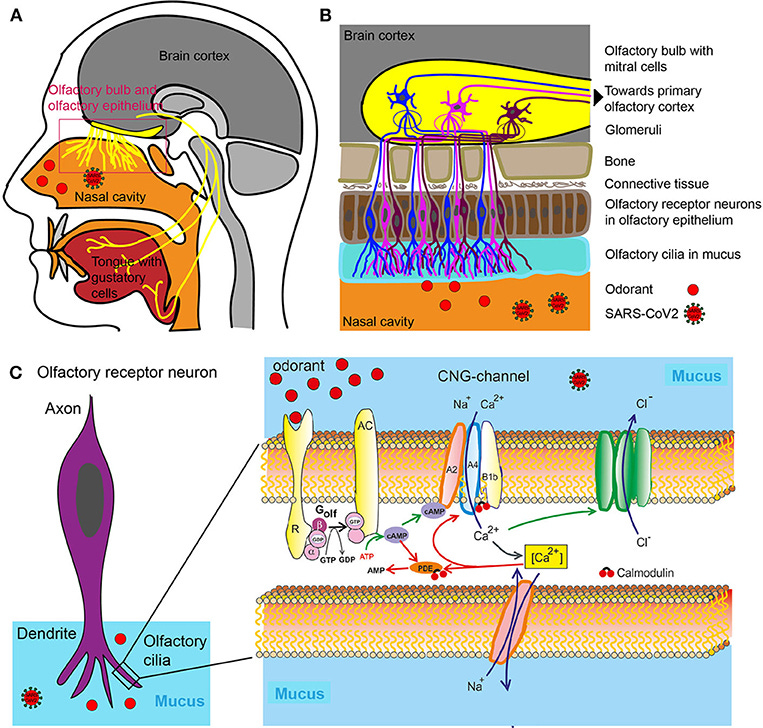
Figure 1. Olfactory system. (A) Head sagittal section showing the olfactory and gustatory systems. (B) Olfactory bulb, olfactory epithelium with olfactory receptor neurons. (C) Left: Olfactory receptor neuron with olfactory cilia. Olfactory receptor neurons are bipolar neurons with a dendrite carrying a crust of sensory cilia. Right: Part of an isolated olfactory cilium illustrating processes upon odorant binding. The green arrows show activating, the red adapting processes. AC, Type III adenylate cyclase; AMP, adenosine monophosphate; cAMP, cyclic adenosine monophosphate; [Ca2+], intracellular Ca2+ concentration; CNG, cyclic nucleotide-gated ion channel; Golf, olfactory G protein; PDE, phosphodiesterase; R, odorant receptor.
“Ageusia is a rare condition that is characterized by a complete loss of taste function of the tongue. It requires differentiation from other taste disorders such as hypogeusia (decreased sensitivity to all tastants), hyperguesia (enhanced gustatory sensitivity), dysgeusia (unpleasant perception of a tastant), and phantogeusia (perception of taste that occurs in the absence of a tastant).”
“Anosmia is the inability to perceive smell/odor. It can be temporary or permanent and acquired or congenital. There are many causes. Neurological causes can include disturbances to the sensory nerves that make up the olfactory bulb or anywhere along the path in which the signal of smell is transferred to the brain. From the olfactory bulb, the signal is further processed by several other structures of the brain, including the piriform cortex, entorhinal cortex, amygdala, and hippocampus.”
“Dysphagia is difficulty in swallowing. Although classified under "symptoms and signs" in ICD-10, in some contexts it is classified as a condition in its own right. ... A wide range of diseases can cause dysphagia. These include:
• Disturbances of the brain such as those caused by Parkinson's disease multiple sclerosis, or ALS (amyotrophic lateral sclerosis, or Lou Gehrig's disease)
• Oral or pharynx muscle dysfunction such as from a stroke
• Loss of sphincter muscle relaxation (termed "achalasia")
• Esophageal narrowing such as from acid reflux or tumors”
“Hyposmia, or microsmia, is a reduced ability to smell and to detect odors. A related condition is anosmia, in which no odors can be detected. Some of the causes of olfaction problems are allergies, nasal polyps, viral infections and head trauma. Hyposmia might be a very early sign of Parkinson's disease. Hyposmia is also an early and almost universal finding in Alzheimer's disease and dementia with Lewy bodies.”